"The one thing we all agreed on was there was a gap of continuity. This patient presents they have a problem -- what’s the next step?"
Karen Butterworth Erban
Emergency rooms all over the country are seeing a huge surge in the number of people being brought in after overdosing on opioids or heroin. There’s no doubt this is a disruption for staff and a strain on resources. But one Connecticut hospital has decided this point of contact with the opioid epidemic actually represents a huge opportunity.
At the emergency department at Backus Hospital in Norwich, as at any other hospital, when someone arrives who has overdosed on drugs, staff will assess the patient and prepare to administer the revival drug naloxone. But Karen Butterworth Erban, who's the Regional Director of Emergency Services, said at Backus one additional thing is happening.
“When that unintentional overdose hits the stretcher, the frontline nurse is calling mobile crisis outreach to say 'I have a patient, they’re in my emergency department, they’re here for overdose,'” Butterworth Erban told WNPR.
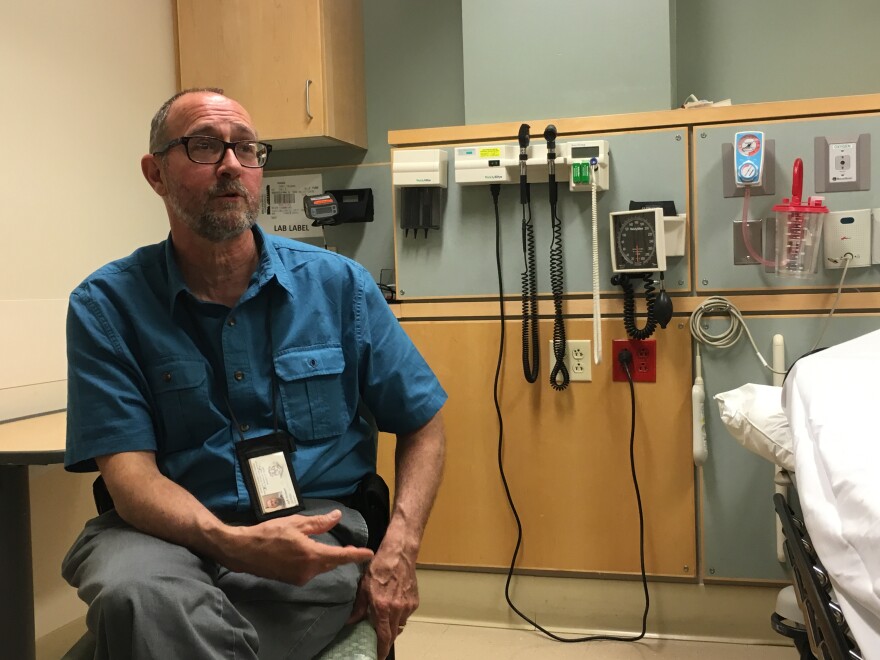
Mobile crisis outreach is a service of the Southeastern Mental Health Authority, a state agency based just 20 minutes away from Backus. And quite often, the person on the other end of that call is supervising clinician Jeff Watson.
“When I’m driving to see somebody in a circumstance like this," Watson said, "I remind myself of all the really great people I know who were very lost in addiction, and have recovered and are doing very well, so I know recovery is possible.”
It’s Watson’s job, after the patient has been revived and stabilized in the ED, to sit with them and ask where they’d like to go from here.
“I remember when we were planning this, I was picturing myself coming in and saying ‘Good morning, you just woke up, you almost died, can we talk?’ That actually doesn’t happen,” Watson said.

In a noisy and sometimes crowded environment, with a patient who can be feeling very sick indeed, it’s best to expect the unexpected. But often, Watson said, there is an opportunity to help them reach out for resources to treat their addiction.
“This is a moment where even in an illness that’s characterized by a lot of denial, where denial is dropped down," Watson said. "You’ve woken up in the emergency room, they’ve told you you were clinically dead or very close to it, and you were brought back. And it’s a moment when sometimes people are more willing to think about what they’re doing than at other times.”

Backus is so far the only hospital in Connecticut taking this approach to overdose.
The genesis of this idea to involve outreach workers in overdose cases came about a year ago, when Butterworth Erban started noticing a whole lot more patients coming to the hospital. She checked the data, and found that indeed the number of overdose cases had doubled. She convened a meeting of local emergency and mental health services. Not everyone had the same priorities. “But the one thing we all agreed on, was there was a gap of continuity," Butterworth Erban said. "This patient presents they have a problem -- what’s the next step? No-one could really articulate what that was, because frankly it didn’t exist.”
In fact, most patients once they were revived with naloxone were simply sent home with just a sheet of paper, listing local addiction resources. Worse still, many would overdose again and come back multiple times. Compounding the problem, being revived with naloxone or Narcan is a pretty unpleasant experience -- leaving the patient in withdrawal, often vomiting and with uncontrollable chills, and not very happy with the nursing staff.
“It’s not the most welcoming interaction you’ll have during your day as a nurse when you have to give Narcan," Butterworth Erban said. "And that used to get frustrating, and that helps to build that stigma and that helps to build the frustration of 'oh so and so’s back again.'”
She said having the backup of a trained mental health or social work professional can also help front line emergency staff to realize that addiction is a disease that needs in-depth treatment.
Chris Burke manages the Southeastern Mental Health Authority, and he has a lot of confidence in the people who are now regularly deployed to the Backus emergency department.
“I have a very experienced team,” Burke said. "They know when to walk away, they know when to say, let’s continue this tomorrow, they know when to say let’s go now.”
This pilot program at Backus has been up and running now for almost a year, and more than 60 overdose patients have been offered the outreach service. Almost 80 percent agree to at least talk to the outreach worker, and 40 percent go on some form of treatment.
Burke said he knows the next step will be to follow through to monitor outcomes. “The data collection is the most cumbersome part," he admitted. "But it’s also, as we move into the 21st century, we know that the data is really, really important. Because we can talk about what we do, I can give you examples of how well it works, but we know that we need to keep the data.”
Dr Jim O'Dea is head of the behavioral health network for Hartford Healthcare, the parent group of Backus Hospital. He said while the opioid epidemic is taking lives every day, it's also worth remembering that many people are entering recovery every day.
"There’s a whole tapestry of resources that we need to make available to our patients," O'Dea said. "But these moments, when people come to the emergency department, and this intervention where we’re connecting people with care right away; I’m completely confident that we’re saving lives."
Backus is so far the only hospital in Connecticut taking this approach to overdose. The Department of Mental Health and Addiction Services says it's in talks with other facilities to see if the program can be expanded elsewhere in the state.